Fighting cancer with immunotherapy has revolutionized treatment for some patients. Emphasize “some.” For most patients, drugs targeting the immune system to attack their tumors aren’t an option.
This could change in the near future. Aided by a deeper understanding of the immune response to cancer, several hundred (repeat: hundred) clinical studies are now pitting cancer immunotherapy drug candidates against many different forms of cancer.
“It’s just an amazing time,” says Dana-Farber Cancer Institute investigator Gordon Freeman. “There’s high energy and enthusiasm among basic scientists, clinical scientists and pharmaceutical companies. The door has been opened and there’s confidence that some of these drugs will work.”
Freeman’s research explained how cancers use molecular signals to avoid attacks from T cells, which act as the soldiers of the immune system by cruising around our bodies and unleashing destructive compounds upon disease cells. To understand the excitement scientists feel, it’s important to understand the different immunotherapy strategies developed from his and others’ discoveries.
It’s just an amazing time. There’s high energy and enthusiasm among basic scientists, clinical scientists and pharmaceutical companies.
Gordon Freeman, Investigator, Dana-Farber Cancer Institute
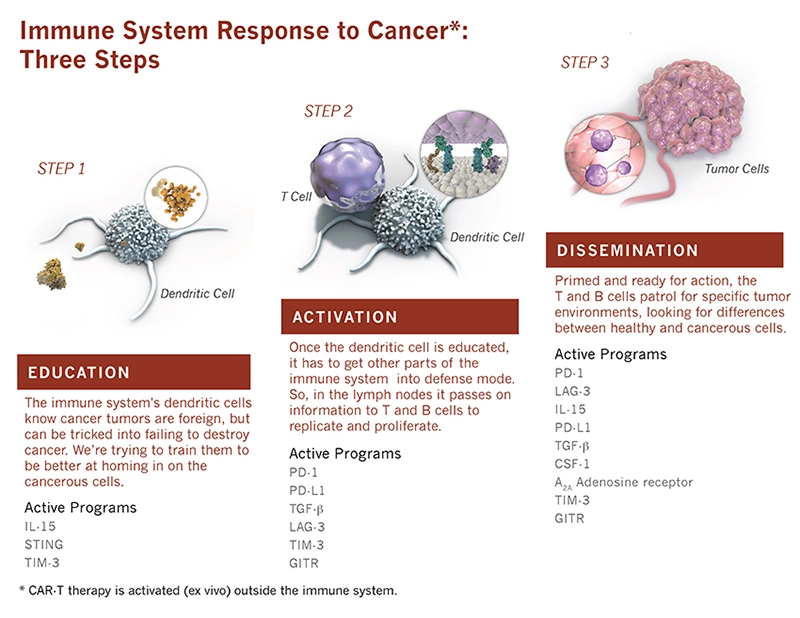
New drugs known as PD-1 inhibitors restore the T cell attack on tumors and have become treatments for types of melanoma, lung and kidney cancers. These new immunotherapies take advantage of the molecular events that can either inhibit or promote immune attacks on cancer. Experts categorize these events into three steps: Education, activation, and dissemination.
In the initial, education step, immune system sentinels called dendritic cells learn about cancer by gathering pieces of dead tumor cells. The dendritic cells then travel to lymph nodes where they present fragments of the tumor to the soldier T cells and B cells, teaching them that this is the enemy to attack, explains Glenn Dranoff, Global Head, Immuno-oncology, at the Novartis Institutes for BioMedical Research.
Then in the activation step, the dendritic cells program the T cells to expand in number and attack the tumor. In the third step, known as dissemination, the T cells and B cells leave the lymph nodes, circulate through the body, recognize the tumors, and mount their offensive.
Unfortunately, tumors find many molecular tricks to evade the immune response to cancer during the process from education to dissemination of immune cells.
Dana-Farber’s Freeman led key discoveries about one of cancer’s favorite tools to trick the immune system and prevent the important activation step. Freeman found that a cell surface protein known as PD-1 can help tumor cells dodge immune responses, essentially serving as an “off” signal to immune cells.
PD-1 belongs to a category of checkpoint proteins that keep the immune system from attacking healthy cells. Among the other proteins serving these checkpoint roles are CTLA-4, TIM-3, and LAG-3. Cancers use these signals, normally found in healthy cells, to disguise themselves as friendly and evade the immune system.
While PD-1 and other checkpoint inhibitors can be effective as solo agents, scientists are learning that when used in combination, two checkpoint inhibitors can be better than one. In advanced melanoma patients, combining PD-1 and CTLA-4 inhibitors provided certain response rates compared to using the CTLA-4 inhibitor alone, according to a study in the New England Journal of Medicine. The U.S. Food and Drug Administration (FDA) in October 2015 approved the combination therapy for the lethal skin cancers.
“This approval is an important result, because it teaches us that addressing different ways that the immune system can be blocked with therapies really can lead to improved clinical outcomes,” Dranoff says.
Ongoing clinical trials pair up checkpoint inhibitors, including compounds that target TIM-3 and PD-1, to explore how these different immunotherapies can work together to block the “off” signals for the immune response. Combining these inhibitors may make them more powerful.
While a bunch of immune system “off” signals may aid tumor growth, many “on” signals that could increase immune responses to tumor cells are weak in cancer patients. You need to strengthen the “on” signals, says Freeman. “There’s a good deal of ongoing research there as well.”
One promising immune-empowering “on” signal, called the STING pathway, begins in dendritic cells activated in the first, educational step of the anti-tumor immune response. In animal models, a potential drug compound triggering the STING receptor not only destroyed tumors but also educated and activated T cell armies to further assault cancer elsewhere in the body.
“The idea is that triggering the STING receptor in the dendritic cells, purposefully and in a controlled fashion, will amplify the ability of the dendritic cells to initiate this educational process,” Dranoff says.
In collaboration with the company Aduro Biotech, Novartis plans to clinically test STING-targeted agents in hopes of igniting immune responses against cancers. The hope would be to eventually use this approach for patients who fail to respond to existing treatments, including other immunotherapies.
“We want to navigate through each of the three steps of the immune response to increase the effectiveness of immunotherapy for more and more patients,” says Dranoff.
This article was developed in collaboration with Dana-Farber Cancer Institute for co-publication on its Insights blog.