On a muggy Thursday in July, Chankey Kumar awoke early, as usual, in the two-bedroom home he, his wife and their infant son share with his parents, aunt, uncle, and two young cousins. He slipped on a blue collared shirt and dress pants — a formality that is unusual where he lives in a working-class neighborhood on the outskirts of Meerut, India, a city several hours north of New Delhi.

After breakfast, he slung a messenger bag over his shoulder, grabbed his motorcycle helmet off a sideboard, and set off for Chhur, one of 69 villages that he visits each month as a health educator for Arogya Parivar, a program launched by Novartis in 2007. The program aims to improve health literacy and the availability of doctors and medicine for some 32 million people living in 14,000 rural Indian villages in a way that is commercially sustainable.
Arogya Parivar, which means healthy family in Hindi, is an example of a “shared value” business model, an approach promoted by Michael Porter and Mark Kramer, professors at Harvard Business School in the US. “For a long time, companies just accepted the world the way it was”, Kramer said. A pharmaceutical company, for instance, would see little point in marketing drugs to the villages that Kumar serves because few people there have access to doctors or enough money to buy medicine. Shared value, on the other hand, is “the idea that societal problems actually represent business opportunity, not cost of doing business”, Kramer said.
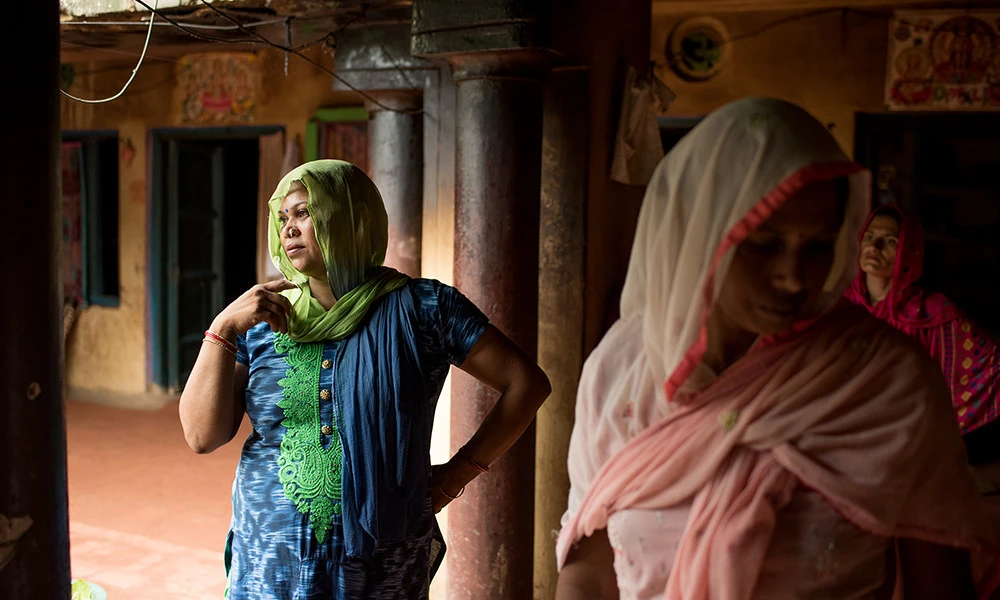
In the case of Arogya Parivar, the need—and the opportunity—is massive: The 70% of Indians who live in poor rural areas account for only 22% of the country’s health expenditures. Most of them make less than USD 5 per day. The health camps Arogya Parivar offers are free and include information on treatment as well as consultations with a doctor, who volunteers several hours of his time in a village in return for exposure to a wider pool of potential patients. In addition, health education sessions that include tips on disease prevention are organized and run by trainers like Kumar, who are recruited locally and understand the village dialect and customs.
Meanwhile, a separate corporate arm of the program peddles inexpensive products for common conditions such as malnutrition and diarrhea to doctors. By 2010, three years into the program, Novartis determined that Arogya was paying for itself by increasing demand for the company’s medicines in the areas it served; the number of doctor visits made by villagers in the locations where the camps were held had tripled.
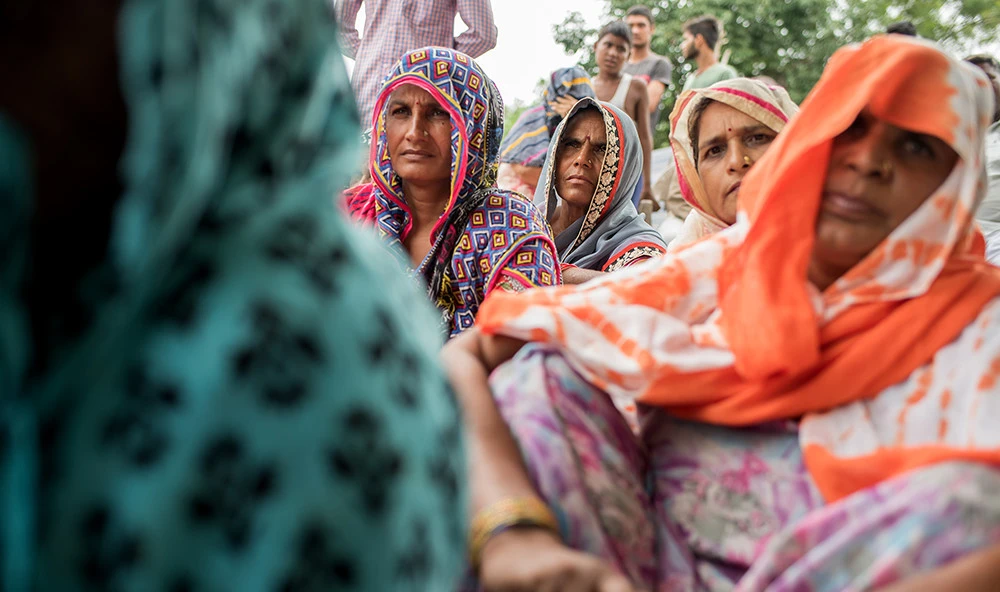
On the ground, however, Arogya Parivar still faces countless challenges—most of which are borne daily by Kumar and the nearly 250 other health educators in the program. Personal beliefs and habits in most villages—such as trusting traditional healers rather than accredited doctors, sharing medications, ignoring nutrition, and open defecation—are ingrained both by culture and circumstance. In the beginning, Kumar’s presentations on hygiene and what to do if you feel sick were met with suspicion and sometimes hostility. “I had never mobilized a crowd”, said Kumar, who is 27 and has been working with the program for four years. “I came home and cried. People would walk out. People would say, ‘We know it better than you. We have busy lives. Don’t bother us’”.
Kumar persisted, eventually gaining the confidence of village leaders and attending a training seminar where he learned to project his voice. Soft-spoken, with serious brown eyes, he began to carry himself with more confidence. That Thursday, passing through a central market on his motorbike, he knocked at the door of a storefront clinic; its resident physician, Sudhir Gupta, emerged and followed him in his car down a bumpy paved road through sugar cane fields to the village of Chhur. In the courtyard of a central temple, Kumar helped villagers set up a makeshift office for the doctor: a folding table and chairs. Then, he jogged out of the courtyard into a neighborhood of open-air houses to round up participants.
In his monthly presentations, he had been urging the villagers to keep their surroundings clean to prevent disease. He pointed to a Mountain Dew bottle in a gutter that encircled the temple. In front of some homes, the gutter was clean; in front of others, litter and cow dung collected, often blocking the drainage and leading to flooding. Standing water attracts mosquitoes and flies, which bring disease. (Chikungunya fever, spread by mosquitos, had plagued Chhur the year before.)
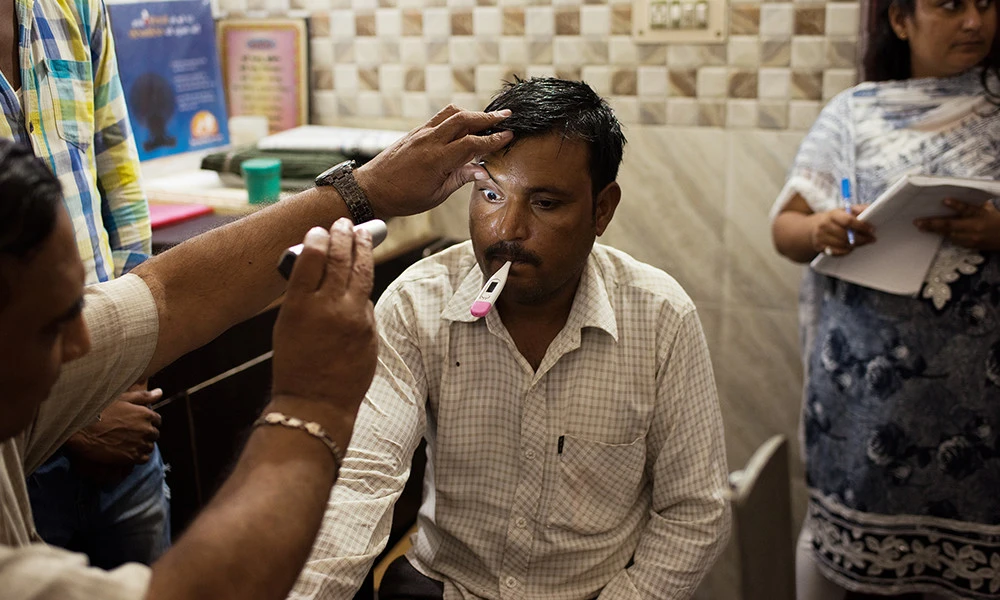
That morning, Dr. Gupta advised a boy with a cold, another whose father feared he had a cognitive impairment, an elderly woman with arm pain, a woman with insomnia and a young man with a back injury. A man with withered legs crawled the length of the courtyard to consult him about stomach pain. For most of them, it was their first visit to a doctor.
From a business standpoint, Arogya Parivar is an obvious success. Novartis plans to expand the program to reach 44 million people in villages across India through health education meetings and health camps by 2022. And it has similar initiatives underway in Kenya and Vietnam.
Lack of proper and robust measurement is an issue for almost every social program in the industry.
Michael Fuerst, Senior Manager of Corporate Responsibility Strategy and Innovation at Novartis
Measuring the social impact of the program, however, has proven more difficult—but perhaps presents a learning opportunity of its own. “Lack of proper and robust measurement is an issue for almost every social program in the industry”, said Michael Fuerst, Senior Manager of Corporate Responsibility Strategy and Innovation at Novartis, who has worked with Arogya Parivar from its inception. “There is a belief in the good deed”— that well-meaning investments will automatically produce positive results. “That’s still assumptive and not based on scientific insight”, Fuerst continued. “I think we should know better”.
To help address this issue, Novartis engaged Richard Laing, a professor at the Boston University School of Public Health in the US, to independently assess a separate program in Kenya called Novartis Access and to recommend a rigorous evaluation method that can be adapted for Arogya Parivar and other healthcare-access programs. He and his fellow researchers will publish the findings from Kenya online where other companies experimenting with shared value can reference them. “We want to bring other companies along and also be more systematic with monitoring and evaluation,” Fuerst says. He sees the study as “a commitment to do better and in the right way”.

In the meantime, Kumar and the others will continue their efforts to gradually improve healthcare access in the communities they serve, often devising their own strategies for engaging local residents. After his visit to Chhur, for example, Kumar drove to the nearby village of Mulehra, where he had organized a street play that he hoped would draw a larger crowd than the roughly 40 people he could typically expect at his sessions.

Just before noon, he and others spread blankets in the swept dirt yard of a village council building and an adjacent primary school. “Where we are sitting it used to be like that”, Kumar said, pointing to an overgrown field next to the school piled with trash. He saw this as a sign that his presentations about proper sanitation were having an effect. As the street play musicians stretched pieces of rubber over the mouths of pots to make drums, a crowd began to gather, eventually numbering more than 100. From out in the street, a row of children peeked over a wall surrounding the yard.

After the performance, Kumar said that the event had unfolded exactly as he’d hoped it would, though a heckler had still interrupted his lesson. “It is good that he spoke in between”, he said. “Because then I can engage with the audience”. The first and perhaps most important step in changing people’s behavior, he knows, is simply getting them to show up.
Additional Resources:
Healthy Family report (PDF 2.0 MB)
A program that combines health education with improved access to doctors and medicines is still going strong, 10 years later.
