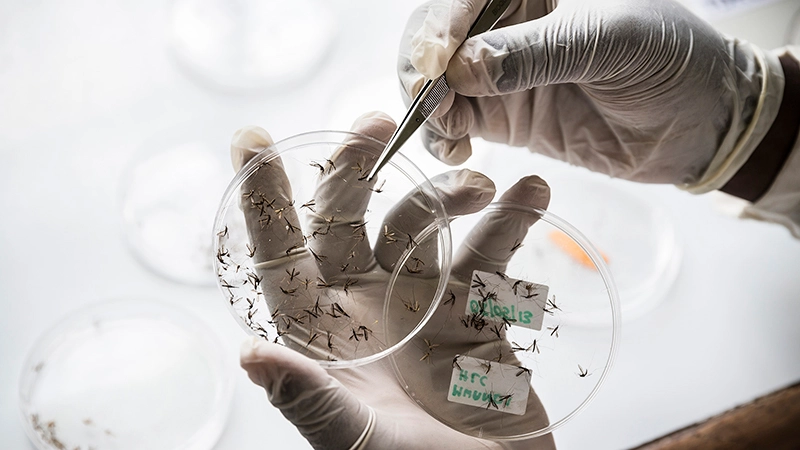

Addressing poverty-related and neglected diseases
Malaria, diarrheal disease, and “tropical” infections such as dengue and visceral leishmaniasis are among many enduring global health challenges that predominantly impact some of the world’s most vulnerable and underserved populations living in lower income parts of the world. The Global Health Disease Area (DA) is discovering novel medicines to help control and, ideally, eliminate these diseases in these populations.
“Some of these diseases have plagued humanity for thousands of years or more,” says Thierry Diagana, who leads the Global Health DA and is California Sites Head for Novartis, Biomedical Research. “We now have the opportunity to apply modern drug discovery technologies and find new solutions to these ancient health problems. Our vision is to invent definitive therapeutics that change the practice of medicine for underserved populations and achieve sustained impact on human health.”
Focused on innovative drug discovery and having advanced small molecule drug candidates into clinical trials, the Global Health DA works in collaboration with philanthropies, academics, governments, and non-profit partners to respond to a broad range of existing and emerging global health challenges.
“I’m proud to work alongside a team of scientists committed daily to helping to solve long neglected, urgent health challenges in global settings,” says Diagana.