The retina, transparent and just half a millimeter thick, contains 10 layers of cells that form a complex signal processor. This biological computer is coated with over 100 million photoreceptive rod and cone cells, the outer tips of which sense light and make sight possible. Damage to these tips, which occurs in genetic diseases such as retinitis pigmentosa, Usher Syndrome, and Leber’s congenital amaurosis, causes blindness that is currently untreatable.
It turns out, however, that a molecular switch controls the growth of the light-sensitive outer segments of cone cells. Botond Roska published his discovery of this switch, two microRNAs, which are small molecules that silence genes, in Neuron in 2014. The microRNAs themselves may have therapeutic potential, says Roska, “but before that there is something simpler, which is to use them to study disease mechanisms.”
Roska’s lab uses mice to model blindness diseases, but mouse retinas and human retinas are quite different. For instance, mice retinas lack a fovea, a tiny, cone-dense region of the human retina that allows for high-resolution color vision. Also, some genetic diseases that cause blindness in humans do not progress the same way in mice.
“We need human models,” says Roska, a neurobiologist at the Friedrich Miescher Institute for Biomedical Research in Basel, Switzerland, a research center affiliated with the Novartis Institutes for BioMedical Research (NIBR) and with the University of Basel.
The first human retina-in-a-dish, created using human stem cells by a team in Japan in 2012, was a pivotal advancement. But these lab-grown retinas could not sense light. So Roska decided to add his newly discovered microRNA switch to a growing retina-in-a-dish. The cone cells began changing. Their outer segments started to grow and function and the cells showed activity in response to light.
“We thought, this is very nice,” says Roska. “Now we can develop a disease model for many human genetic retina diseases in a dish.”
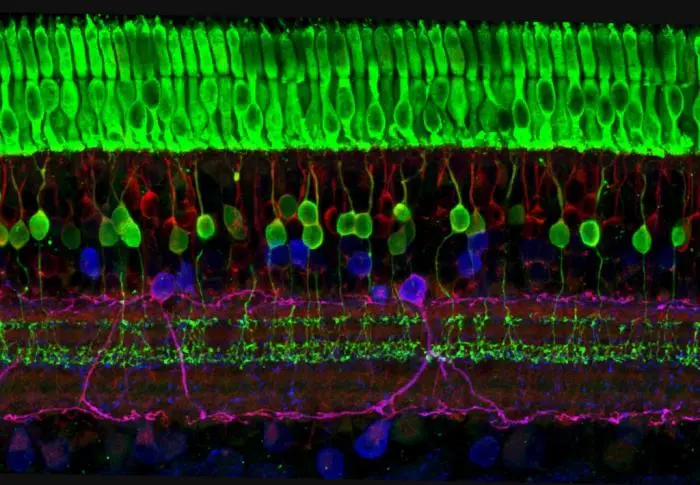
Layers of nerve cells of the retina, including the top layer of photoreceptors (green). Courtesy of Wei Li, National Eye Institute, National Institutes of Health.
Roska’s recent efforts have been focused on building retina-in-a-dish models from the cells of real patients. He and collaborators in Switzerland begin by taking a skin sample from a person with a gene mutation associated with a disease, such as retinitis pigmentosa. With the right biochemical cues, these skin cells are coaxed back into stem cells, called induced pluripotent stem (iPS) cells, that become the building blocks of the model retinas-in-a-dish.
Additional cues, including modulation of Roska’s microRNAs, prod the iPS cells to transform into different types of retina cells, and to self-assemble into a living, light-sensing model retina.
“These lab-grown retinas are obviously not an eye, but they have a lot of the rudiments of an eye, so we can use them to learn a lot,” says Tewis Bouwmeester, Head of the Developmental and Molecular Pathways department at NIBR in Basel, who is collaborating with Roska to build new models of blindness diseases. The project supports NIBR’s exploration of molecular signaling pathways that drive organ development – and the misfires that cause disease – to gain insights that could lead to new potential therapies, in this case for inherited causes of blindness.
Roska hopes that these retina-in-a-dish disease models will begin to show symptoms. “The treatment will come when we can clearly see the disease in a dish and learn how to treat it,” he says.
This dual effort to understand and cure is emblematic of Roska’s work.
“He is absolutely dedicated to fundamental discovery, but he also is interested in turning that understanding into ways to treat blindness diseases,” says Bouwmeester.
Bouwmeester is also collaborating with Roska on a simpler way to model blindness diseases in rods and cones grown without the rest of the retina. Creating a lab-grown retina is time-consuming, so their goal is to build cultured cell models that can be produced quickly and efficiently in large volumes.
If the work is successful, these cell models could be used to screen potential therapies to see which works best to repair the damage caused by disease. From there, promising drug candidates can be tested in the more realistic retina-in-a-dish model.
Read “Vision Hacker” to learn more about Roska.



