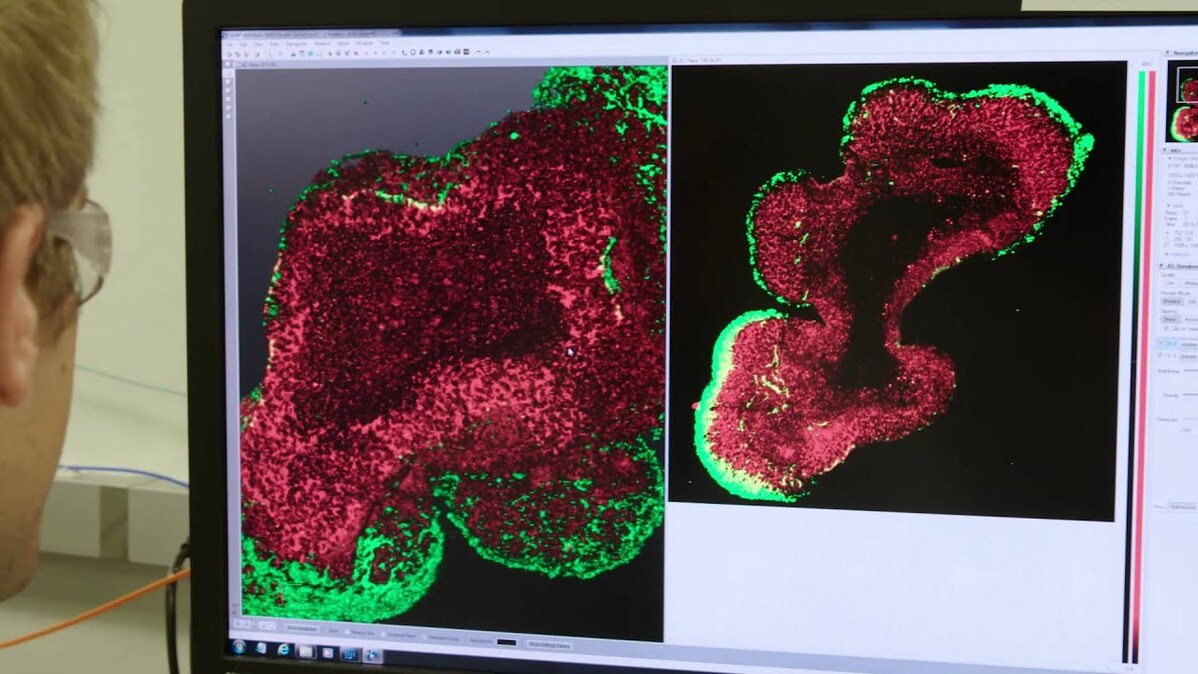
Max Salick reaches into an incubator in his lab and pulls out a dish with small, grayish blobs floating in a deep pink fluid. He places the dish gently under a microscope and turns on a camera. One of the blobs flashes up on a nearby screen, magnified. Close up, it starts to look vaguely familiar, almost like a tiny brain.
And it is, sort of. In reality, that blob is a miniature, organ-like structure made from human cells that mimics key features of the brain's outer layer of gray matter, the cortex.
It may not look like much, but “brains in a dish” like this one may offer researchers their best bet yet for demystifying developmental and degenerative brain disorders like Alzheimer’s, tuberous sclerosis complex (TSC) and autism, as well as discovering new ways to treat them.
 VIDEO
VIDEO
Mutations wreak havoc
Salick is part of a team within Neuroscience at the Novartis Institutes for BioMedical Research that’s building brains in a dish. The scientists have started by focusing on TSC, a devastating genetic condition that the Tuberous Sclerosis Alliance estimates afflicts nearly 1 million patients worldwide. TSC patients have mutations in one of two genes, TSC1 and TSC2. Normally these genes work together to turn off a growth-boosting signaling pathway called the mTOR when it’s not needed. When mutated, though, the genes can’t do their job, and affected cells grow when they’re not supposed to.
It may not look like much, but “brains in a dish” like this one may offer researchers their best bet yet for demystifying developmental and degenerative brain disorders...
"Patients with these mutations get growths all over their bodies — their skin, their kidneys, the heart, their lungs," says Salick, who is a postdoctoral researcher. "But the biggest impact comes from benign brain growths called tubers."
The tubers form because neurons arrange themselves improperly during development. Those misalignments wreak havoc with normal brain function. "Patients with TSC can have cognitive delays, epilepsy, autism and other neurological disruptions," Salick explains. "The brain symptoms are the biggest detriment to quality of life in TSC." And while there are tuber-shrinking drugs on the market, there are no treatments that correct all of the defects seen in the brains of TSC patients.
Origins of an organoid
TSC and other degenerative or developmental brain disorders pose a unique challenge for researchers — it's nearly impossible to study them while they develop in living brains. These “brains in a dish,” however, let researchers get pretty close.
To grow one, Salick and his supervisor Ajamete Kaykas turn to an unexpected source of cells: the skin. In the lab, the team biologically re-programs skin cells from TSC patients into induced pluripotent stem (iPS) cells. These cells are in a nearly embryonic state and can grow into just about any cell type in the body. Because they're generated from a patient's cells, the iPS cells harbor the same TSC1 or TSC2 mutations causing that patient's disease.
Using a cocktail of proteins and small molecules — and with the help of a room-sized cell culture robot he affectionately calls "the neuron factory" — Salick then guides the iPS cells to become nerve cells. He also uses the patient-derived cells to grow what scientists call a cerebral organoid.
To grow one, Salick and his supervisor Ajamete Kaykas turn to an unexpected source of cells: the skin.
With these patient-derived “brains in a dish” — along with “healthy” ones Salick is generating using cells from individuals without TSC — the team has created an advanced lab-based representation of what happens in the developing brain of a person destined to develop TSC.
"With organoids we can study the interactions of multiple cell types in something close to a living model," says Kaykas, who leads the team. "There is no other system that lets you get as close to modeling a human brain."

First glimpses
Although much of Salick's work over the last year has focused on refining the methods for growing organoids as consistently as possible, with similar size and structure, he's already starting to turn up some interesting results.
"It's all very preliminary, but at very specific time points we start to see changes in how the TSC organoids grow," he says. "There are size differences, the neurons are bigger, and the layers are different as well. And they appear to form growths that look like tubers."
Soon, he and Kaykas hope to start examining how neurons in TSC “brains” fire, and also start to look for possible treatments from among the millions of compounds in the Novartis drug discovery library.
"If you can show that what you're seeing in the organoids matches what's seen in the brains of patients," Kaykas muses, "then you potentially could run a trial in a dish and test an experimental drug in a human cellular model before going to the clinic, rather than in a mouse."



