Did you know cardiovascular disease (CVD) affects hundreds of millions of people worldwide?1 Yet approximately 80% of CVD, including heart attack and stroke, is preventable.2
Knowing the risk factors associated with CVD is an important first step in helping to prevent it. While some factors can’t be changed, such as age, gender, and family history, others are modifiable, meaning that you can take steps to change them. Modifiable risk factors for CVD include high blood pressure, smoking, diabetes, obesity and elevated levels of low-density lipoprotein cholesterol (LDL-C).3,4
One genetic driver of CVD that you may not have heard of before is lipoprotein(a) – often shortened to Lp(a) and pronounced L-p-little-a. When elevated in the blood, it increases the chances of having a cardiovascular event such as a heart attack or a stroke.5 But what is Lp(a) exactly, and how does it impact CVD risk?
What is Lp(a)?
Lp(a) is a type of fat particle, somewhat similar to cholesterol. It is normal to have Lp(a) in the blood.6,7
Are elevated levels of Lp(a) bad for health?
Elevated levels of Lp(a) in the blood can cause the build-up of a fatty deposit in the arteries called plaques, known to be an underlying cause of CVD.6-10 If a plaque ruptures, it can cause a cardiovascular event such as a heart attack or a stroke.11
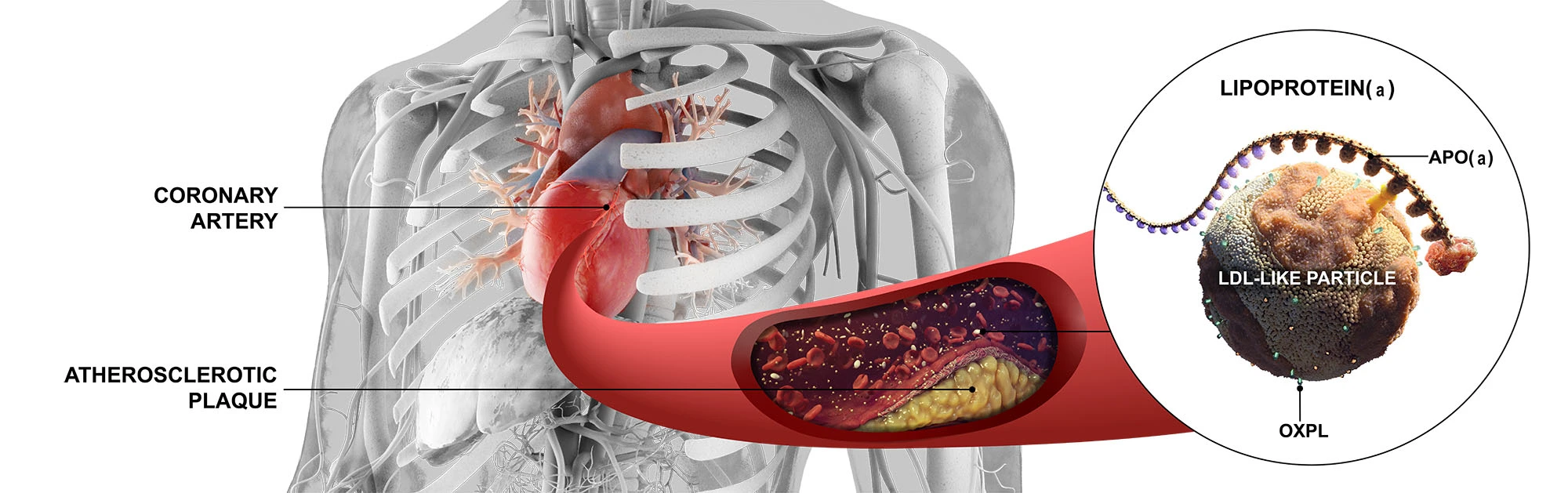
It is important to know that elevated Lp(a) increases the chances of a cardiovascular event, regardless of the presence of risk factors like hypertension, high cholesterol, diabetes, diet and exercise.5,10,12-17 In fact, people with elevated Lp(a) could be approximately three times more likely to have a heart attack compared to those with normal levels.13
While having elevated levels of Lp(a) increases a person’s likelihood of CVD, this does not guarantee they will develop it. 18
What causes levels of Lp(a) to be elevated?
Lp(a) levels are genetically predetermined – that is, passed down from parent to child. If one parent has elevated Lp(a) levels, a person would have a 1 in 2 chance of also having elevated Lp(a) levels. Lp(a) levels cannot be significantly changed through lifestyle changes such as diet or exercise.10,17,19-21
How common is elevated Lp(a)?
Elevated Lp(a) is common – approximately one in five people worldwide have it but won’t know unless they get tested.17,22
Elevated Lp(a) levels can affect anyone but may be more common in certain ethnic groups.23 Around 20% of the global population – that’s about 1.5 billion people! – have elevated Lp(a) levels, but many people who appear healthy may not know they are at risk.17
What is an “elevated” level of Lp(a)?
The higher the level of Lp(a) in the blood, the greater the chance of having a cardiovascular event.18 Generally, Lp(a) levels in the blood are considered low risk if they are less than 30 milligrams (mg) per deciliter (dL) or 75 nanomoles (nmol) per liter (L). Levels higher than this are believed to increase the risk of developing CVD, and levels greater than 50 mg/dL or 125 nmol/L are considered elevated.17
In general, levels do not change very much over a person’s lifetime, though they can vary in women.17,24,25 This is because Lp(a) levels tend to increase during menopause.25
How are Lp(a) levels tested?
Knowing if a person has elevated Lp(a) is needed to fully understand their overall risk of cardiovascular events and to make the best-informed decisions with them on their overall care.26 Lp(a) should be measured at least once in all adults,25,27 using a routine, non-fasting blood test as part of general heart health checks.28-30
It is especially important to test Lp(a) in people with:25,27,29,31
- A cardiovascular event in the last year,
- A cardiovascular event at a young age,
- More than one cardiovascular event,
- A family history of cardiovascular events at a young age.
In most people, only one test is needed to determine Lp(a) levels and whether it increases a person’s overall CVD risk.18
What treatment options are available for people with elevated Lp(a) levels?
Although no specific treatments are available, testing for Lp(a) is still critical to fully understand a person’s overall cardiovascular risk, how closely they need to be monitored and how intensely to manage other modifiable risk factors such as cholesterol and hypertension.26
If a person’s Lp(a) levels are elevated, they can work with their doctor to evaluate their overall CVD risk and develop an appropriate plan of action.
Can lifestyle changes improve Lp(a) levels?
Because Lp(a) levels are genetically predetermined, they can’t be significantly changed through lifestyle changes like diet and exercise.10,17,19,20 However, diet and exercise can positively impact other risk factors and so should be considered as part of a person’s action plan to manage their overall cardiovascular risk.
Novartis continues to lead the way in educating about cardiovascular health and elevated levels of Lp(a).



