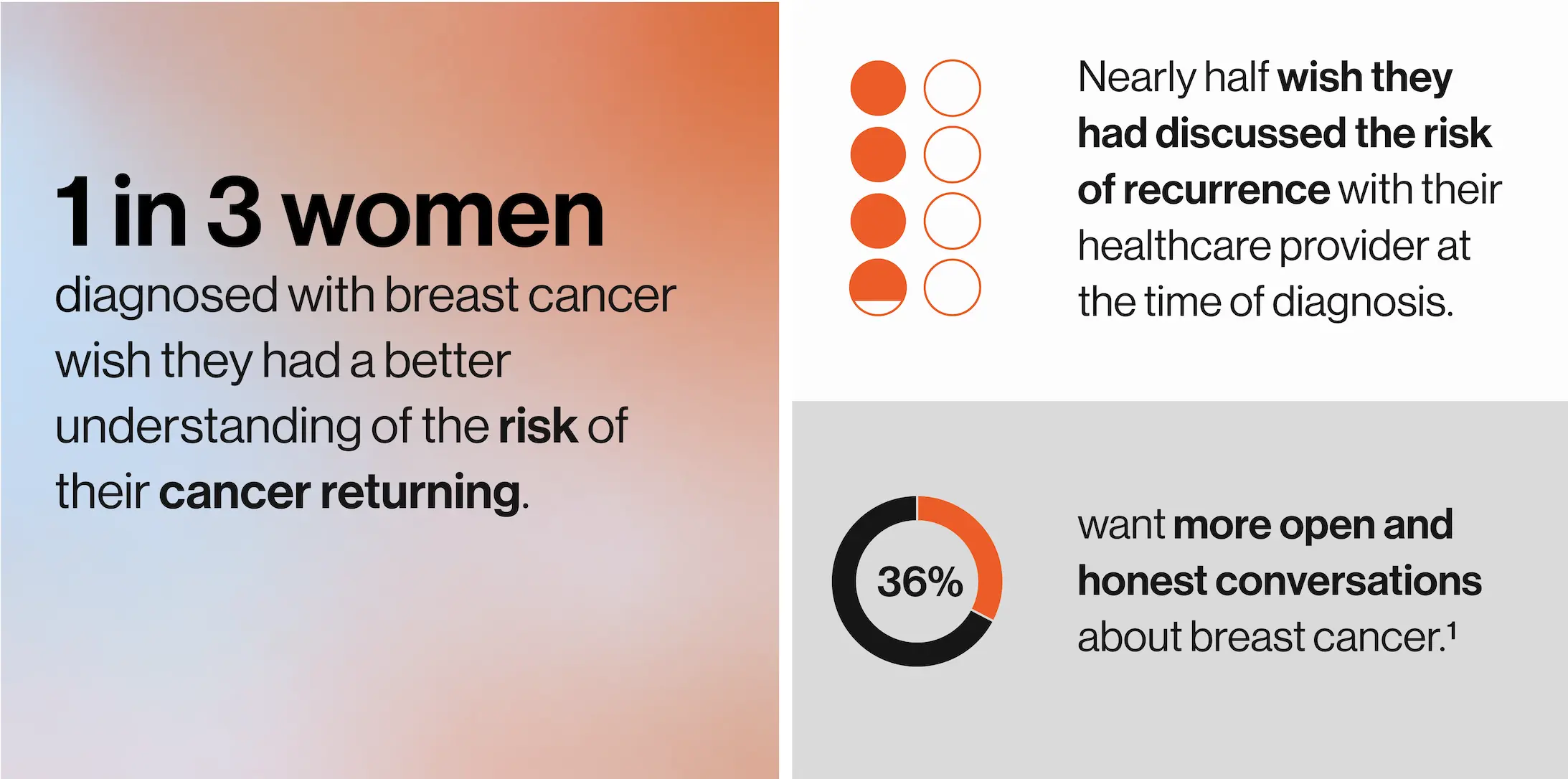
For many women, the end of breast cancer treatment is described as a turning point, bringing mixed emotions and questions about if cancer could come back.
The worry does not always arrive loudly. It can show up as a pause before a routine scan, a tightness in the chest at a follow-up appointment, or a question that forms in the mind but never quite makes it to the doctor's office. The concern of breast cancer returning may not be a single moment — but a backdrop, present in ways both large and small, sometimes for years after treatment ends.
To better understand how women experience and navigate breast health, Novartis partnered with The Harris Poll to develop the Breast Health & Experience Index, a first-of-its-kind survey of more than 3,000 women in the United States, both with and without breast cancer.
The findings paint a clear picture: for women living with or beyond a breast cancer diagnosis, concerns about recurrence are common, deeply felt, and too often unaddressed.
What the Index Revealed
These findings point to a need for shared decision-making, where patients and care teams work together, earlier and more openly, to navigate what comes next.
Below, we explore common insights about breast cancer recurrence and the kinds of questions many women say they wish they had been able to ask sooner.
1. What does it mean if breast cancer comes back?
When breast cancer returns after initial treatment, it’s called recurrence. Even after surgery and other treatments, it’s possible for some cancer cells to remain in the body and grow again months or years later.2 This is different from developing a new, separate cancer, which requires its own evaluation and care.
When breast cancer does return, it can come back in a few different ways:3
- Locally: In the same breast or nearby area (also known as a local recurrence)
- Regionally: In the lymph nodes near the breast
- Distant: In other areas of the body, such as the bones, liver, or lungs (also known as distant recurrence or metastatic breast cancer)
2. Does recurrence risk change based on cancer stage?
Yes. In early breast cancer (stages 1-3), life after treatment often involves an awareness that the cancer could return, with risk levels based on characteristics of the cancer, including stage.
Some types of early breast cancer are driven by hormones in the body, and as a result, the possibility of the cancer coming back can persist for many years after treatment ends.4 Hormone receptor-positive, HER2-negative (HR+/HER2-) is the most common type of breast cancer, affecting about 7 out of 10 people diagnosed with the disease.5
Current research shows that for people with HR+/HER2- early breast cancer, in the first 3 years after initial treatment:6
- Up to 1 in 9 people with Stage 2 will have their cancer come back
- Up to 1 in 5 people with Stage 3 will have their cancer come back
While these numbers offer general guidance, the chance of breast cancer returning differs from person to person. Importantly, there may be treatment options available that can potentially reduce the risk of recurrence. This is why early and ongoing conversations about treatment options can help provide a clearer understanding of a patient’s individual recurrence risk and what steps may help reduce it.
3. What additional factors shape individual risk?
Every person’s risk is different and can be influenced by several factors that their healthcare team considers, including:7-9
- Cancer type and hormone receptor status
- Cancer stage, size, and grade at diagnosis
- Number of lymph nodes involved
- Age and menopausal status
- Overall health and medical history
- Genetics and family history of breast cancer

This is where open conversations matter most. By discussing personal risk factors directly, patients and providers can build a follow-up plan that is tailored and empowering.
Questions to consider asking a healthcare provider:
- “Based on my diagnosis and treatment, what does my personal risk look like?”
- "Are there additional treatments or monitoring steps we should consider based on my risk factors?"
- “How often should I check in, and what follow up care should I expect?”
- “Who should I contact if I have questions or notice something new?”
4. What symptoms should you watch for to know if breast cancer has returned?
Most new symptoms after breast cancer treatment are not a sign that cancer has returned. But some changes are worth noting and discussing with a healthcare provider, including:10
- Changes in the size, shape, or color of your breast
- New lumps, swelling, or rashes on the body
- Persistent bone, chest, or joint pain that doesn’t improve
- Unexplained symptoms that last for weeks or keep getting worse
Keeping a symptom diary can make it easier to share concerns clearly with your provider. Reaching out to your care team is never a bother. If something doesn’t feel right, speaking up matters.
5. The worry is real. So is the power of talking about it.
It’s completely understandable to feel worried when thinking about the possibility of breast cancer returning. For many people, that concern does not disappear when treatment ends. It becomes part of the landscape after a diagnosis.
The barrier to conversation is not always a lack of information. For care teams, something as simple as asking, "What are you most worried about right now?" can open the door.
While no one can control everything, many people find comfort in focusing on steps they can take to stay engaged in their care and support their overall well-being, including:
- Keeping up with follow‑up appointments and recommended scans, even when they’re feeling well
- Taking prescribed treatments as directed and speaking with a healthcare provider if challenges come up
- Paying attention to changes in the body and documenting them for timely evaluation
- Prioritizing physical, mental, and emotional health in ways that feel manageable
Moving Forward, Together
The Novartis Breast Health & Experience Index makes clear that women are not asking to be shielded from difficult information. They are asking for earlier, clearer information, and a genuine partnership with their care team.
At Novartis, we are committed to supporting people throughout their breast cancer journey by listening and providing the resources that help women feel informed and empowered at every stage. Because when patients and care teams can talk openly about recurrence risk, the path forward becomes clearer for everyone.
To learn more about breast cancer risk of recurrence, connect with support groups and explore resources to help guide conversations with your healthcare team, visit UnderstandeBCRisk.com.
Methodology
The research was conducted online in the United States by The Harris Poll on behalf of Novartis among 2039 US women age 18 or older (“US Women”) and 1001 US women age 18 or older diagnosed with breast cancer (“Breast Cancer Patients”). The survey was conducted June 11–23, 2025.
Data are weighted where necessary by age, race/ethnicity, region, education, marital status, household size, employment, household income (not included for women diagnosed with breast cancer), and smoking status to bring them in line with their actual proportions in the population.
Respondents for this survey were selected from among those who agreed to participate in our surveys. The sampling precision of Harris online polls is measured by using a Bayesian credible interval. For this study, the sample data is accurate to within ± 2.5 percentage points for US women and ± 4.4 percentage points for breast cancer patients using a 95% confidence level. This credible interval will be wider among subsets of the surveyed population of interest.
All sample surveys and polls, whether or not they use probability sampling, are subject to other multiple sources of error which are most often not possible to quantify or estimate, including, but not limited to coverage error, error associated with nonresponse, error associated with question wording and response options, and post-survey weighting and adjustments.